Viral exanthema in childhood
This article was written by Dr. Pleimes, a specialist in pediatrics, dermatology, and allergology.
Learn more about Dr. Pleimes here.
The term exanthema refers to a skin rash that typically affects larger areas of the body.
What are the causes and triggers of exanthema?
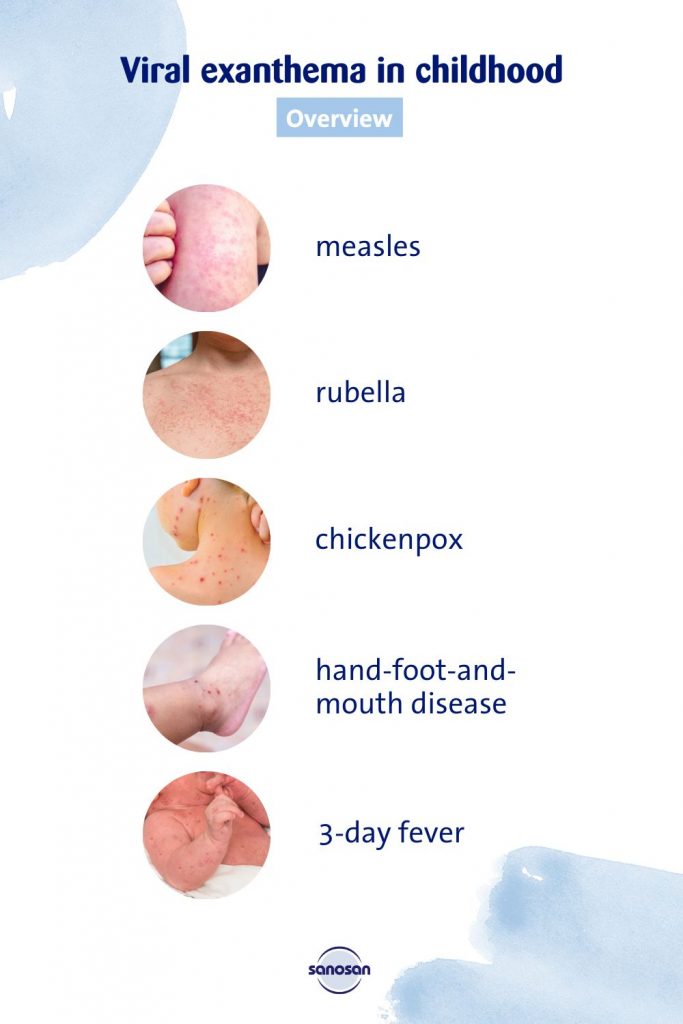
An exanthema can have different causes. In childhood, viral infections are often the cause. Some pathogens, such as chickenpox or measles, very often trigger a typical exanthema and usually lead to the typical course of the disease in unvaccinated people, which is why these, along with other infectious diseases such as rubella, ringworm or 3-day fever, are counted among the classic exanthema diseases in childhood.
However, many, many other mainly viral pathogens also trigger exanthema. However, not everyone who has the infection also gets an exanthema. And not every exanthema looks the same in everyone affected. This also explains why some children only get a cold and others also develop an exanthema. The vast majority of exanthema in children falls into the category of non-specific exanthema. This means that we do not know the exact pathogen, but we do know that the rashes are generally harmless. Most exanthema is only present for a short time and disappears by itself.
However, some infections can also lead to a stimulation of the immune system that lasts longer than the actual infection. These paraviral or parainfectious exanthema can often last longer and sometimes last for many weeks or even months. There are a number of other rashes that we can assign to a specific appearance of the individual spots, but where we do not know the triggers for certain.
In addition to the skin, the mucous membranes can also be affected in many forms of exanthema. This can manifest itself in various types of spots in the oral mucosa or on the child’s throat.
What are the effects of exanthema in childhood?
Various exanthema diseases not only lead to a rash, but can also lead to persistent problems for individual sufferers or problems that occur over time. We therefore try to vaccinate all children against these diseases at an early stage in order to avoid possible side effects.
Rubella
For example, rubella can lead to joint inflammation or inflammation of the brain and, particularly in the case of infection during pregnancy, to serious damage to the unborn child.
Measles
Inflammation of the central nervous system can also occur in children with a measles infection. In some cases, this takes a chronic course, which sometimes only occurs years later, but cannot be treated with our current medical measures.
Chickenpox
Even with chickenpox, severe courses are possible, in which inflammation of the meninges or the central nervous system also occurs. A special feature of chickenpox viruses is that they remain in the body of the infected person and can be reactivated later in a certain area. This can be triggered by stressful situations with reduced immune defense of the body. As only a certain area of the skin is usually affected and the affected areas on the trunk of the body are usually distributed in a belt shape (on the arm and leg in a line), this is referred to as shingles. In the chickenpox vaccination, a weakened but still viable virus is inoculated in order to achieve a sufficient defense of the body. We know that shingles can also occur in vaccinated children, but this happens much less frequently overall. Dermatologists have a particular interest in ensuring that some of their patients are vaccinated against chickenpox as early as possible according to the recommendations, as children with a sensitive skin barrier, such as those with neurodermatitis or certain keratinization disorders of the skin (ichthyosis), can get very severe chickenpox infections and these can then leave many scars on the body.
How can I tell if my child has an exanthema and what it is?
Some of the classic childhood diseases/exanthem diseases already have a very typical course. In vaccinated children, however, we no longer see measles, rubella and chickenpox, which belong to these very specific courses.
Measles
Unvaccinated children who have contracted measles, for example, first have a fever, cough, runny nose and conjunctivitis. After a brief improvement without fever, a new phase of illness occurs with swelling of the lymph nodes, renewed fever and usually a reduced general condition. This results in the typical measles exanthema, in which there are usually large patches, some of which merge.
Rubella
In contrast, rubella is characterized by a very fine-spotted rash and the children usually feel much better. It is very typical of chickenpox that the rash is itchy and there are many different stages of individual spots. Small new red spots with blisters and older as well as crusted spots appear side by side. It is also typical that the hairy head is also affected.
Hand-foot-and-mouth disease
If blistering occurs in vaccinated children, similar to what we see with an initial chickenpox infection, this is often caused by an infection with enteroviruses or Coxsackie viruses. In a classic course, there is the so-called hand-foot-and-mouth disease, which leads to the formation of blisters with underlying redness in the area of the palms of the hands, soles of the feet, in the diaper area, on the mouth and oral mucosa. However, individual members of the virus group also trigger more extensive rashes in individual children, in which the entire arms or legs and sometimes even the trunk of the body can be affected.
3-day fever
Another very common exanthema in children is the 3-day fever, the so-called exanthema subitum. The name comes from the fact that most children with 3-day fever have a very high fever for about 3 days with a relatively good general condition. As the fever subsides, some of those affected then develop a 3-day fever rash, sometimes lasting only hours to 1-3 days, which appears as a bright red, fine-spotted exanthema. The disease is also triggered by a virus from the herpes group. Almost all children have been infected at least once by the age of around 3 years. This also shows that the classic rash does not always occur, but only in individual children.
What treatment options are there for exanthema?
The treatment of most exanthema is usually purely symptomatic, which means that the virus itself is not treated, but at most the accompanying itching or perhaps more severe inflammation, for example if an additional bacterium should settle on an open spot. Only in the case of rashes caused by bacteria, such as scarlet fever, will your pediatrician prescribe an additional antibiotic if necessary.
When does it become dangerous and when can I relax?
Fortunately, most rash/exanthema diseases in children are harmless and the children are usually relatively well. They are only slightly or moderately affected during the disease phase. Warning signs of a severe course are a severely impaired general condition of the child and rashes on the skin that are palpable and do not fade, i.e. lose their color, when an affected area of skin is pressed together with a stable glass of water, for example. This is a sign of vascular involvement in the skin with accompanying bleeding and can occur, for example, in the context of a severe bacterial infection. Rashes that lead to extensive, continuous reddening of the body or skin detachment similar to burns, open lips or an open oral mucosa are also warning signs, all of which should be clarified by a doctor immediately in these extremely rare cases.
In most cases, however, exanthema is harmless, the children are only slightly affected and everything disappears by itself within a few days.








